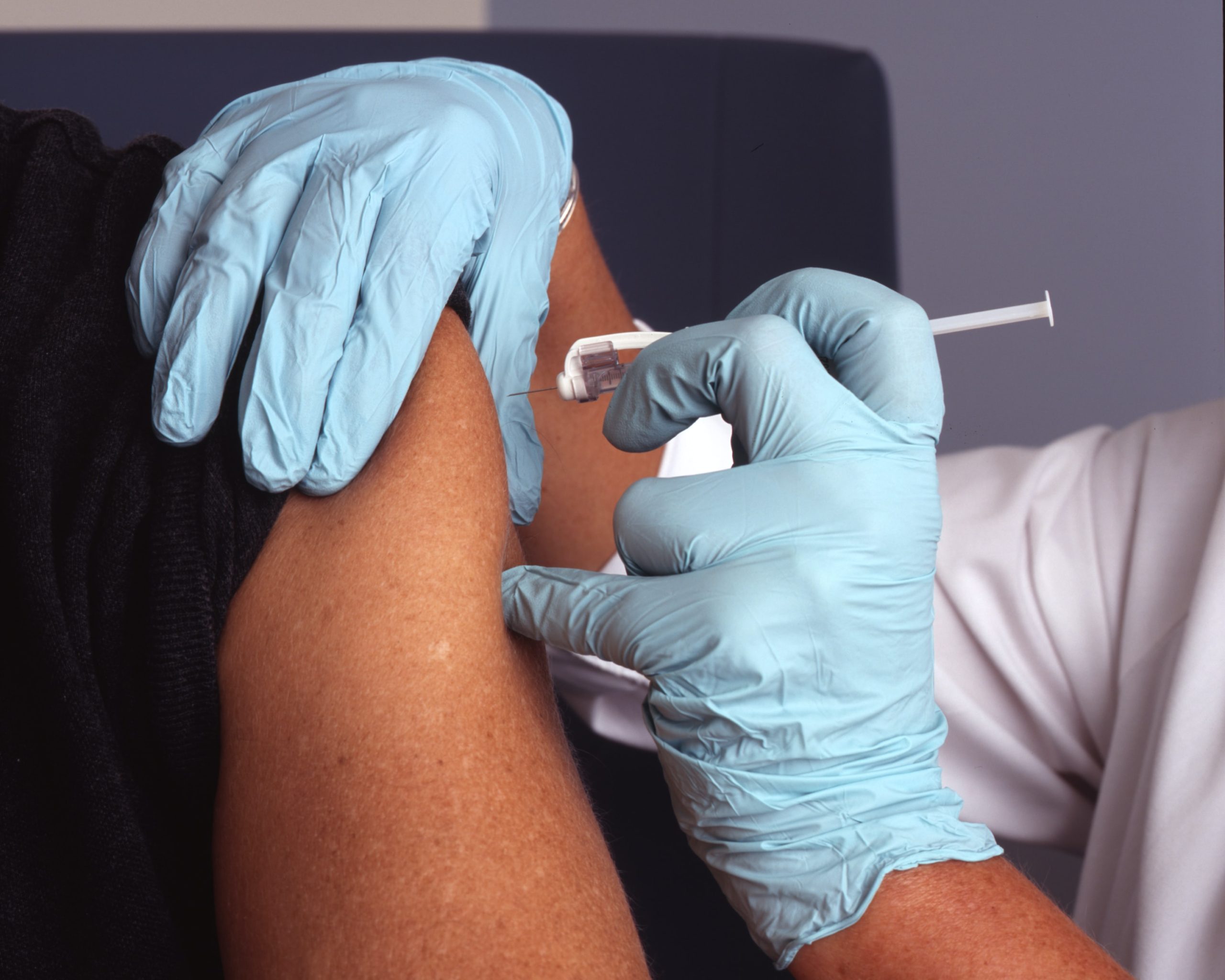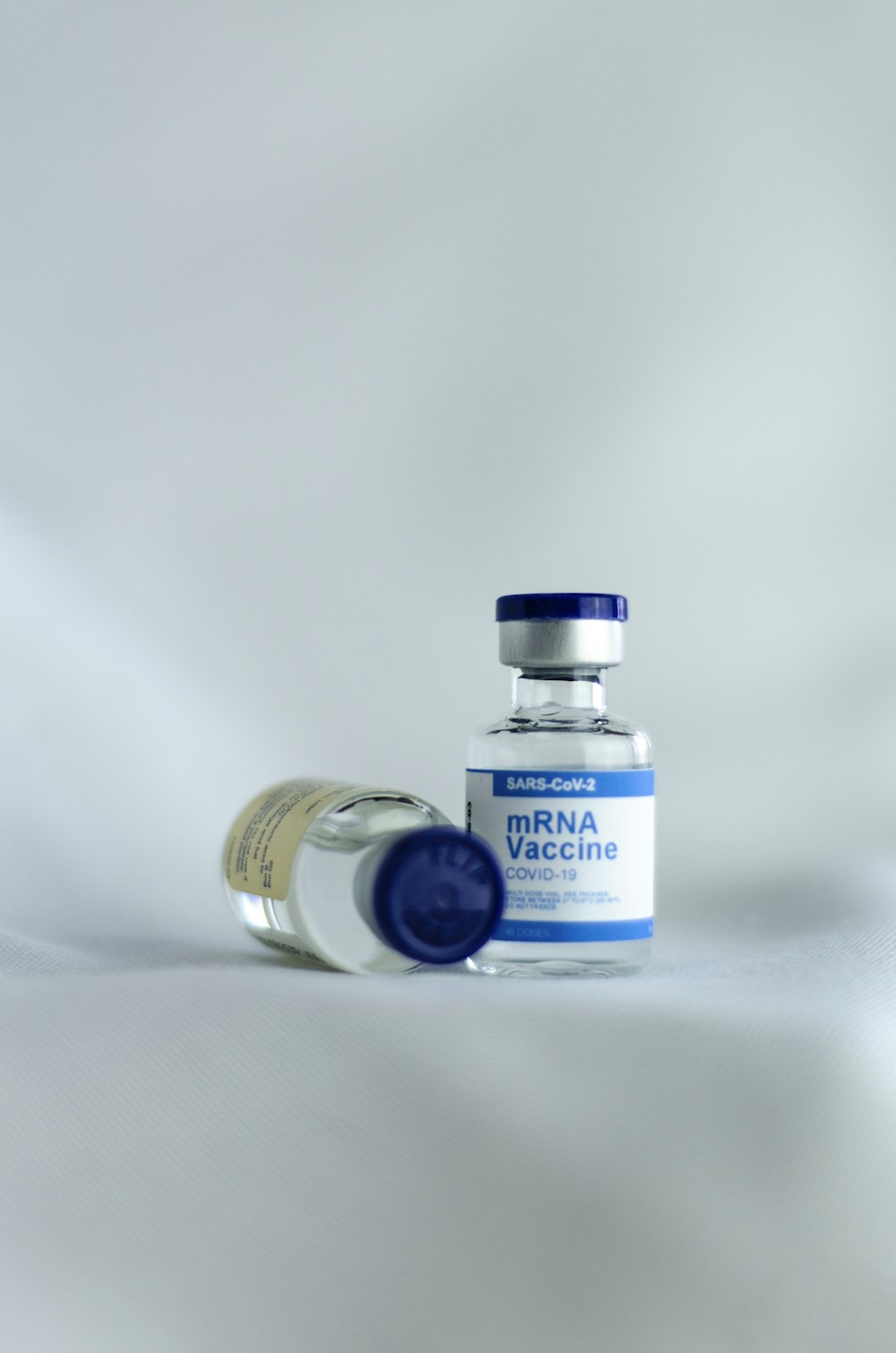
What is mRNA, and why are mRNA vaccines so attractive?
The completion of the Moderna and BioNTech-Pfizer vaccines against the SARS-CoV-2 virus is a remarkable feat –from conception to widespread clinical use in one year. This does not mean, however, that the concept behind this vaccine is completely new. Although messenger ribonucleic acid (mRNA)-based vaccines have long been affected by a lack of funding, this past year’s breakthrough in mRNA vaccine research represents only the beginning of a new era of vaccine technology. What is mRNA and why are mRNA vaccines so attractive? mRNAs are the middlemen in the central dogma of science: that is, genes in the form of DNA are first transcribed into mRNAs, and then translated into proteins, which ultimately carry out the cellular functions necessary for life. As such, all living human cells already contain the molecular machinery necessary to read an mRNA and produce the protein it encodes. mRNA vaccines harness this system to artificially and transiently produce antigens (molecules that stimulate the immune system and cause the body to recognize the molecule as a harmful entity). For example, the Pfizer-BioNTech and Moderna mRNA vaccines encode the spike protein of the SARS-CoV-2 virus. This is one benefit of mRNA vaccines that allows them to generate broad immune protection against a disease. Secondly, the development of genetic sequencing technologies allows scientists to determine the full genetic code contained within viruses, and these sequences can then be turned into mRNA artificially to generate a vaccine for specific viral antigens. Compared to traditional vaccines which depend on using cells to grow viruses which are then attenuated, killed, or turned into fragments, the process of producing mRNA vaccines is relatively fast, cheap, and can be done without the use of cells. Finally, mRNAs themselves can act as an adjuvant (a component of a vaccine that generally boosts immune responses), since cells contain mechanisms that recognize mRNA and induce inflammatory responses. However, a drawback of this is that an inflammatory response may be induced toward the mRNA itself, rather than the antigen that the mRNA is meant to produce. With the rise in funding for mRNA vaccine research, scientists can begin to address this and other open questions and continue improving on this technology. Altogether, mRNAs represent a highly time and cost-effective way to generate novel vaccines.
A brief history of mRNA vaccines
The possibility of recruiting the body’s own cells to make proteins from artificially introduced mRNAs was first suggested as early as 1990. Dr. Jon A. Wolff and colleagues published a seminal report in Science showing that RNA injected into mouse muscle successfully induced the production of their corresponding proteins. While this was not necessarily considered vaccination because the goal was not to induce an immune response, this work demonstrated that it is entirely possible to introduce foreign mRNA into a host animal, and that the mRNA would survive inside cells and reliably produce the protein it encodes. This is the foundation for mRNA vaccines. There also remained questions about how to effectively deliver the mRNA into cells without the immune system mounting a response against and degrading the mRNA itself before it had the opportunity to work as a vaccine. In addition, the field was restricted by lack of funding and public interest. Despite these hurdles, researchers such as Dr. Katalina Kariko intensively studied the biology of RNA, and spearheaded efforts to further develop mRNA vaccine technology. She and Dr. Drew Weissman made the breakthrough discovery of how to prevent the recognition of vaccine mRNAs by human immune cells, thereby allowing the mRNA to enter into cells and work as intended. Dr. Pieter Cullis, whose primary work focuses on generating lipid nanoparticles, later collaborate with Drs. Kariko and Weissman to package mRNA vaccines into lipids. This keystone research laid some of the groundwork for the founding of both Moderna and BioNTech in the early 2010s.
Applications of mRNA vaccines
Infectious Diseases: Since the seminal work from Drs. Wolff, Kariko, Weissman, and Cullis in the 1990s and early 2000s, the use of mRNA vaccines not only against viruses, but also against bacteria and cancer have been explored using animal studies. These studies use a number of different methods of delivery in mice, rats, rabbits, ferrets, pigs, and rhesus macaques to protect against a wide variety of diseases. As a proof of concept, one group reported that antibodies against the Rabies virus were strongly induced in mice given an mRNA vaccine that encoded for a viral component present on its surface. Aside from the SARS-CoV-2 vaccines developed in response to the COVID-19 pandemic, there are several clinical trials either completed or in progress, aiming to use mRNA vaccines as a method of protecting against infectious diseases that currently have no cures –HIV-1, Rabies, Zika, and Influenza. Trials assessing the efficacy of an HIV-1 vaccine conducted by Argos Therapeutics, Massachusetts General Hospital, and McGill University Health Center have shown results ranging from no effect to moderate effect but have largely been unsuccessful in inducing a sufficient antiviral immune response. The push continues, however, as other groups continue to conduct HIV-1 vaccine trials, and companies such as Moderna begin trials for Zika and Influenza viruses.
Cancer: The flexibility of mRNA vaccines makes it an excellent approach to developing anti-cancer vaccines as well. Since cancer is highly heterogeneous and can evolve over time, much like infectious diseases, they cannot all be treated using the same approaches. Therefore, the possibility of fine-tuning the immune response to specifically target a protein being expressed by cancer cells is highly intriguing and could lead to new breakthroughs in both prevention and treatment. Currently, the majority of clinical trials have focused on melanoma, although vaccines against other cancers, including acute myeloid leukemia, chronic myeloid leukemia, multiple myeloma, mesothelioma, glioblastoma, and many others are in development. Several completed studies have reported limited negative side effects, and control of the growth of cancer to varying degrees. Impressively, a metastatic melanoma study revealed significantly higher rates of long-term survival in recipients who responded well to the vaccine. There still remains much to learn about how mRNA vaccines work, how they should be delivered, and how they affect different cells of the immune system.
Conclusion
One silver lining of the COVID-19 pandemic has been the enormous efforts and funding put towards refining mRNA vaccine technology. This cost-efficient and fast method of producing safe and effective vaccines not only means that there is potential to further reduce infectious disease but also in the prevention or treatment of cancers, and possibly even in autoimmune disease treatment. Overall, the advent of mRNA vaccines represents an exciting new era in both preventative care and treatment of diseases.
References
Buranyi, S. (2021, June 3). The mRNA vaccine revolution is just beginning. WIRED UK. https://www.wired.co.uk/article/mrna-vaccine-revolution-katalin-kariko
Government of Canada (July 30, 2020). The long road to mRNA vaccines. CIHR. https://cihr-irsc.gc.ca/e/52424.html
Kariko, K. et al. Incorporation of pseudouridine into mRNA yields superior nonimmunogenic vector with increased translational capacity and biological stability. Mol. Ther. 16, 1833–1840 (2008).
Pardi, N. et al. mRNA vaccines —a new era in vaccinology. Nat Rev Drug Discov 17, 261–279 (2018).
Wolff J. A. et al. Direct gene transfer into mouse muscle in vivo. Science 247, 1465-1468 (1990).
Brito, L. A. et al. Self-amplifying mRNA vaccines. Adv. Genet. 89, 179–233 (2015).
Routy, J.-P., Nicolette, C. Arcelis AGS-004 dendritic cell-based immunotherapy for HIV infection. Immunotherapy 2, 467-476 (2010).
Jacobson, J. M. et al. Dendritic cell immunotherapy for HIV-1 infection using autologous HIV-1 RNA: a randomized, double-blind, placebo-controlled clinical trial. J. Acquir. Immune Def. Syndr. 72, 31–38 (2016).
Gandhi, R. T. et al. Immunization of HIV-1-infected persons with autologous dendritic cells transfected with mRNA encoding HIV-1 Gag and Nef: results of a randomized, placebo-controlled clinical trial. J. Acquir. Immune Def. Syndr. 71, 246–253 (2016).
Martinon, F. et al. Induction of virus-specific cytotoxic T lymphocytes in vivo by liposome-entrapped mRNA. Eur. J. Immunol. 23, 1719–1722 (1993).
Conry, R. M. et al. Characterization of a messenger RNA polynucleotide vaccine vector. Cancer Res. 55, 1397–1400 (1995).
Hoerr, I., Obst, R., Rammensee, H. G. & Jung, G. In vivo application of RNA leads to induction of specific cytotoxic T lymphocytes and antibodies. Eur. J. Immunol. 30, 1–7 (2000).
Kyte, J. A. et al. Immune response and long-term clinical outcome in advanced melanoma patients vaccinated with tumor-mRNA-transfected dendritic cells. Oncoimmunology 5, e1232237 (2016).
Krienke, C. et al. A noninflammatory mRNA vaccine for treatment of experimental autoimmune encephalomyelitis. Science 371, 145-153 (2021)
Annie Pu
Latest posts by Annie Pu (see all)
- An AI-generated picture worth a thousand words - October 2, 2025
- The old and the new: combining artificial intelligence with traditional medicine - May 13, 2025
- mRNA vaccines: Leading a new era of medicine - October 4, 2021